
Why Foods You've Always Eaten Are Suddenly Making You Sick
What's Secretly Sabotaging Your Gut — And Making Your Perimenopause So Much Worse?
You've been eating the same things for years. The glass of wine on Friday night. The aged cheese on your charcuterie board. The spinach smoothie every morning because someone told you it was healthy.
Nothing changed—except that now your body is reacting to all of it.
Flushing. Headaches. Rashes. Gut disturbance that comes out of nowhere. If you are doing everything "right" but your body feels like it is constantly sounding an alarm, you aren't crazy. You are likely experiencing a massive shift in your neurochemistry and gut microbiome.
If histamine intolerance in perimenopause is something you've never heard of, by the end of this post, you'll know exactly what changed in your body, why your safe foods are suddenly triggering you, and the first three steps to calm your system down.

What Histamine Actually Has to Do With Your Hormones
Histamine isn't just an allergy chemical that makes you sneeze in the spring. Your body produces it, and your immune cells release it as part of normal biological signaling.
The problem in perimenopause is what estrogen fluctuation does to the system that's supposed to keep histamine balanced.
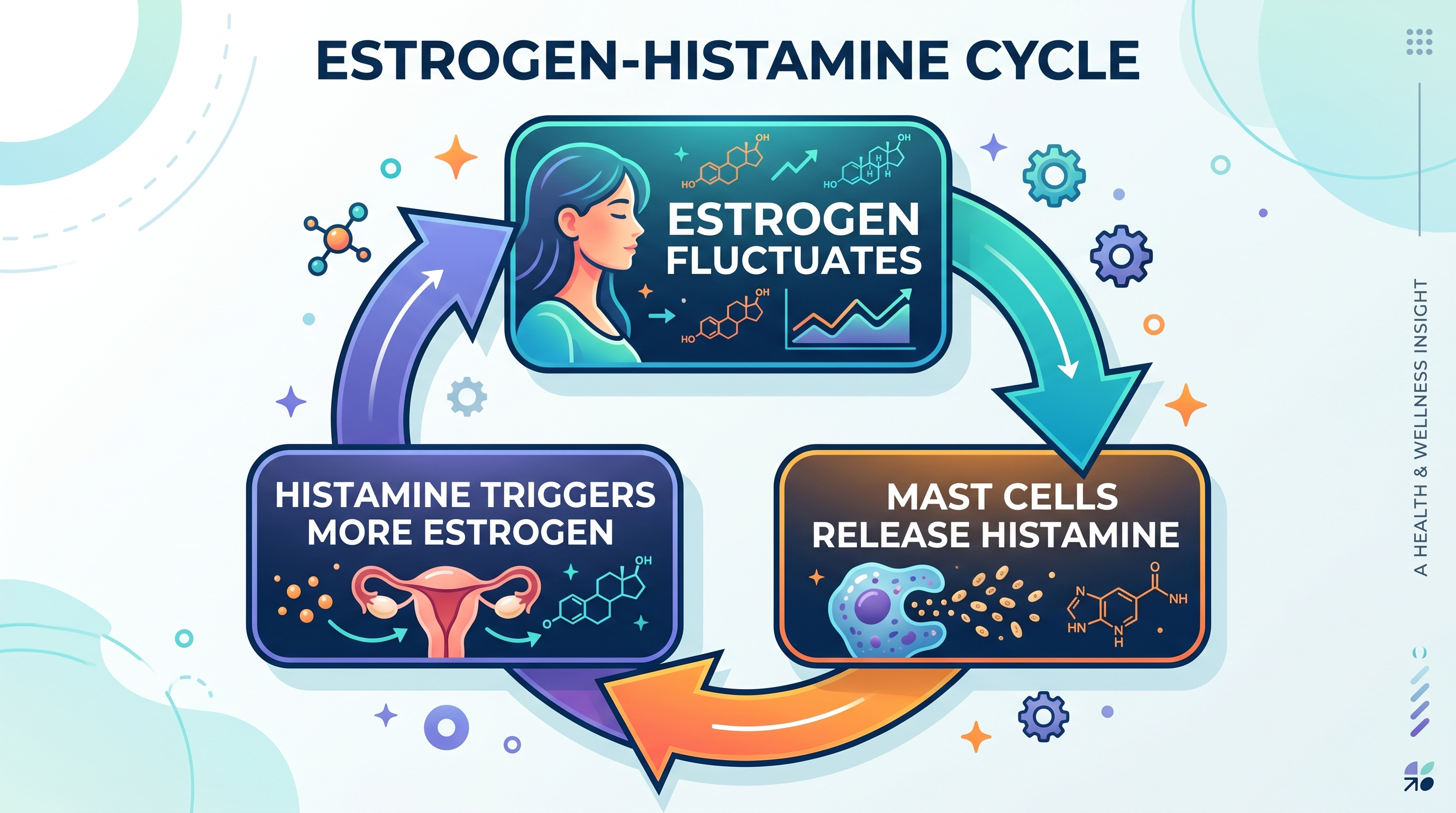
The Hidden Estrogen-Histamine Loop
Here's the connection most doctors miss when evaluating women over 40:
Estrogen activates mast cells—the immune cells that release histamine into your bloodstream.
Histamine then signals your ovaries to produce more estrogen.
When estrogen is stable, this loop stays perfectly controlled.
When estrogen lurches high and crashes low—as it naturally does in perimenopause—the loop spirals out of control.
The result? Foods that never triggered a reaction before are now overwhelming a system that's already overloaded. This isn't a new allergy. It's an existing loop that lost its primary regulator.
The "Healthy" Foods Quietly Running That Loop
When your histamine bucket is full, you don't need to eat junk food to make it overflow. Some of the biggest triggers will surprise you because they carry massive health halos.
Leftovers and Meal Prep
Leftovers are a hidden trigger most women never connect to their symptoms. Histamine levels in cooked protein rise with every hour it sits in the fridge. The meal-prepped chicken you cooked on Monday is a completely different chemical food by Wednesday.
Wine and Aged Cheese
Wine and alcohol are among the highest histamine foods there are. Worse, alcohol directly blocks the enzyme that breaks histamine down in your gut—so one glass of wine now does the damage that three used to do because your clearance capacity has dropped. Similarly, aged cheese (Parmesan, aged cheddar, and gruyère) concentrates histamine the longer it ages.
Spinach and Fermented Foods
Yes, spinach is naturally high in histamine regardless of freshness. If you've been adding it to smoothies daily and wondering why you feel flushed or itchy, this is worth paying attention to. Furthermore, fermented foods like kombucha, sauerkraut, and kimchi are incredible for a healthy gut microbiome, but they are massively high in histamine. For a woman whose clearance system is compromised, the benefit may not outweigh the load right now.
Why Your Body Can't Clear It Like It Used To
There's an enzyme called diamine oxidase (DAO) that breaks down dietary histamine in your gut lining.
When your gut is inflamed, your microbiome diversity is low, or you've been under chronic stress, your natural DAO production drops. Less DAO means dietary histamine accumulates in your bloodstream. This is exactly why symptoms that used to require a massive trigger now happen with one glass of wine or yesterday's leftover salmon.
How to Support Your DAO Enzyme
The good news is that you can support DAO production through food. Fresh apples, onions, and capers are high in quercetin—a natural compound that stabilizes mast cells and helps your gut manage the histamine load.
For high-histamine days, I keep a specific, professional-grade quercetin formulation on hand. Because supplement quality matters—especially when your gut is already reactive—I don't recommend buying this on Amazon.
You can find the exact third-party tested brand I use with my patients inside my private dispensary.
Shop the Quercetin in My Fullscript Dispensary →

What to Do Starting This Week
You don't need a restrictive, miserable elimination diet to start getting information about your body.
Keep a simple food-symptom log for two weeks. Don't track calories or macros. Just track what you ate and what your body did within two hours (e.g., skin flushing, gut bloating, sudden headache, brain fog). Patterns will emerge much faster than you expect.
While you're watching for those patterns, make these four simple swaps:
Fresh fruit eaten same-day (mango, pear, apple) instead of dried or stored fruit.
Fresh protein cooked and eaten immediately instead of multi-day leftovers.
Kale or chard instead of spinach in your salads and smoothies.
Olive oil and lemon instead of vinegar-based dressings.
Take the Next Step: Find Your Gut Saboteur
Your food sensitivities in perimenopause aren't random. Fluctuating estrogen levels disrupt your body's ability to clear histamine. By making simple swaps—like choosing fresh protein over leftovers—you can lower your histamine load and finally calm your nervous system.
Do you want to know exactly what is driving your specific symptoms?
Take the Free Gut Saboteur Quiz. In 2 minutes, you will find out exactly which gut pattern is driving your perimenopause symptoms—and get a personalized starting point for your first week of healing.
Take the Free 2-Minute Gut Saboteur Quiz →
Source: Hrubisko M et al. Histamine Intolerance — The More We Know the Less We Know. Nutrients. 2021. DOI: 10.3390/nu13072228
Affiliate Disclosure: Dr. Stacey Denise is a participant in the Amazon Services LLC Associates Program. I may earn a small commission if you purchase through my links at no extra cost to you. I only recommend products I personally use or would recommend to my patients.
Published: April 2026 | Dr. Stacey Denise | The Neuroaesthetic MD™
